What сan doctors offer? What can doctors help you with? What are they ready to prescribe? Pills, injections, surgical operations, and… a mobile app. And no, these aren’t the countless fitness apps for tracking steps or sleep movements. These are genuine digital medicine products whose effectiveness in treating a range of disorders is already considered proven.
And of course, there are already success stories:
“By week three, my sleep efficiency had improved noticeably. By week five, I was sleeping more consistently than I had in years. The mechanism works. But it requires you to trust a process that feels wrong before it feels right,” – says a patient who used the Sleepio app to overcome insomnia she’d suffered from for over seven years.
“…[The] program has opened my mind in the sense that I can shift my focus to something more important aside from the pain,” – shares a user of the VR device for fighting chronic pain.
The number of such reviews — both glowing and critical — can easily be multiplied, but the story of “digital medicine” being accepted by doctors, regulators, and patients is far from complete. Let’s try to tell it.
What is Digital Therapeutics?
The commonly accepted term for medicinal apps – digital therapeutics – emerged ten years ago, in 2015, when Saeid Sepah and colleagues from Stanford and the University of California, San Francisco proposed one of the first formal definitions in the Journal of Medical Internet Research. They described evidence based digital therapeutics as “evidence-based behavioral treatments delivered online that can increase accessibility and effectiveness of healthcare.”
Just two years later, a specialized organization appeared: the Digital Therapeutics Alliance, which defines DTx as digital therapeutics software intended to treat or alleviate a disease, disorder, condition, or injury by generating and delivering a therapeutic intervention that has a demonstrable positive therapeutic impact on a patient’s health.

The main difference between DTx and wellness or health apps is that DTx must demonstrate effectiveness through clinical evidence, obtain regulatory approval for use, and target a specific medical disorder or disease rather than general well‑being.
In other words, a digital therapeutics solution differs from traditional medicine in nothing but its digital essence. Here, the analog of the active substance is cognitive-behavioral therapy — a type of psychotherapeutic intervention that lends itself much better to algorithmization than many other treatments.
How it works: The Sleepio app helps people overcome insomnia
The program was launched in 2013 by insomnia specialist Colin Espie and former insomnia sufferer Peter Hames. It is based on cognitive behavioural therapy for insomnia (CBT‑I) techniques and personalized algorithms.
The full course is designed to last at least six weeks.
In the first stage, the user explains their problem to the program by filling out a questionnaire and describing the nature of their sleep difficulties. Next, the program introduces the general structure of therapy and explains the main causes of insomnia, as well as the habits and behaviours that sustain it. In the following stage, the user begins keeping a sleep diary and tracking their daily routine.
Every morning, the user logs into Sleepio and notes the time they went to bed, how long it took to fall asleep, how many times they woke up during the night, when they got up for the day, and how they rate their sleep quality. The app can also sync data from wearable devices, such as Fitbit, Apple HealthKit, and others.

During the second week, the virtual “Prof” starts adjusting the user’s behaviour: the sleep window is narrowed to increase sleep efficiency, and Stimulus Control is introduced (the rule that the bed is only for sleep and sex, breaking the habit of lying in bed and “suffering”). The user receives a set of rules: return to bed only when sleepy; get up at the same time every day; and avoid or strictly limit daytime naps.
In the third week, the user learns to address negative thoughts and fears (“I won’t be able to fall asleep,” “I’m in for torture tonight”) through cognitive restructuring.
In the fourth week, the user learns relaxation techniques and anxiety management.
In the following week, the program combines behavioural regulation, cognitive restructuring, and elements of healthy sleep hygiene—such as avoiding bright light, caffeine, strenuous exercise, and screens before bed.
In the final week, the user learns how to maintain the results and prevent relapses, receiving an action plan for bad nights and instructions on how to return to a stable sleep routine.
Does Digital Therapy Help? And For What Exactly?
The benefits of digital therapeutics were first highlighted in clinical studies over 10 years ago. The Prevent app (now known under the Omada brand) is designed to treat a medical disorder by correcting habits in people with prediabetes, a common chronic disease.
Diabetes and weight issues remain the main areas of DTx application according to digital therapeutics market data. By 2025, 19 digital therapeutics clinical trials had already been conducted to verify DTx effectiveness in improving diabetes patients’ conditions, and a meta-analysis confirms their efficacy as clinically validated digital therapeutics.
There are many other examples of digital therapeutics: digital therapy has proven effective against insomnia (in 2012, clinical trials showed SleepioRx’s effectiveness); in treating addictions (in 2017, the Food and Drug Administration approved approved digital therapeutics for treating alcohol, cocaine, and marijuana dependence); and in managing chronic pain (specifically for back pain relief) .
Moreover, digital therapeutics for mental health have shown great promise, including specialized digital therapeutics for depression that help patients manage symptoms through structured evidence-based therapeutic interventions.

In the US, the FDA views DTx as a type of mobile medical application and software as medical devices; in Germany, the DiGA system operates, where digital health products can receive provisional status. Similar registries for digital therapeutics services exist in the UK, South Korea, and France.
Advocates of digital medicines say they deliver therapeutic results at unprecedented scales, especially amid shortages of psychiatrists. The Digital Therapeutics Alliance explicitly positions DTx as an answer to doctor shortages and burnout. DTx products also hold great development potential — adaptive algorithms allow them to create individual tracks for better health outcomes.
Digital Therapeutics Market Snapshot
- The DTx market: $ 9.6 billion (2025)
- Projected growth: $ 75.4 billion by 2034
- Largest market: North America, fastest-growing: Asia Pacific
- Key challenge: data security and privacy concerns
- Major opportunities: shift toward preventive and value-based care
- The top five players: Otsuka Holdings, Teladoc Health, Virta Health, Omada Health, and Pear Therapeutics — 75% of the market
Source: Global Market Insights
Risks and Forecasts
Skeptics don’t dispute that DTx can work, but they doubt its degree of effectiveness. They point out that most digital therapeutics clinical trials involved relatively small numbers of participants.
From a regulatory perspective, digital therapeutics remain somewhat in a gray area: it’s unclear how to classify and reimburse DTx — as a medicine, device, service, or supplement.
In the Digital Therapeutics Alliance review Year in Review: Digital Therapeutics in 2023 and Beyond, 2023 was called “a rollercoaster” for the industry. The main limitation remains the gap between innovation and implementation. The digital therapeutics landscape is indeed entering a phase of tough selection, where primarily products with strong clinical evidence will survive.
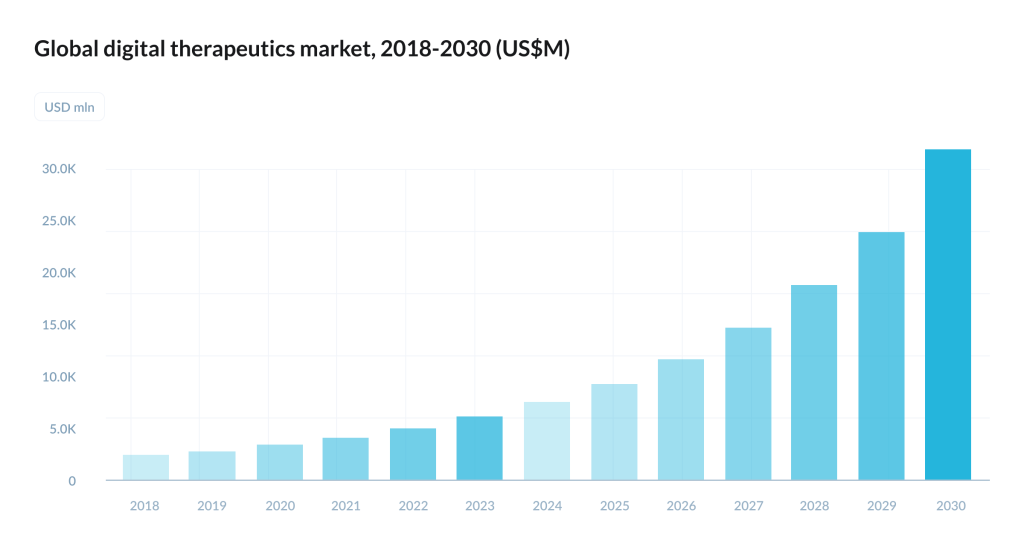
According to industry analysts, further digital therapeutics market development will be accompanied by consolidation and M&A: research reviews describe DTx as a sector where large players will absorb smaller ones, and survivors will be those who can combine clinical effectiveness and a clear reimbursement path .
On the 5–10 year horizon, digital therapeutics will likely take root in segments with existing sustained clinical effects: insomnia, diabetes, mental health, chronic pain, and rehabilitation.


